Get Instant Callback
Didn’t Find What You Were Looking for! Get a call back from Expert Dentist
Cavities causing pain or sensitivity? Clove’s expert, tooth-coloured fillings stop decay and restore your teeth with a natural, comfortable finish.


Is tooth pain, sensitivity, or a visible cavity making it hard to eat or focus?
At Clove, we understand how quickly a small cavity can turn into constant discomfort affecting your meals, sleep, and daily routine. Our dentists use gentle, modern techniques and tooth-coloured fillings to stop decay early, relieve pain, and restore your tooth’s natural strength and appearance.
Book a consultation for fast, comfortable, worry-free care.
Dental fillings repair tooth damage caused by cavities, cracks, or minor injuries. Your dentist removes the decayed part of the tooth and restores the space with a strong, tooth-coloured material that blends naturally with your smile.
A filling is a quick, single-sitting procedure that usually takes less than 30 minutes, yet it plays a major role in protecting the tooth for the long run. By sealing the area and preventing bacteria from entering, fillings stop decay from progressing, relieve sensitivity, and restore normal chewing comfort and strength.
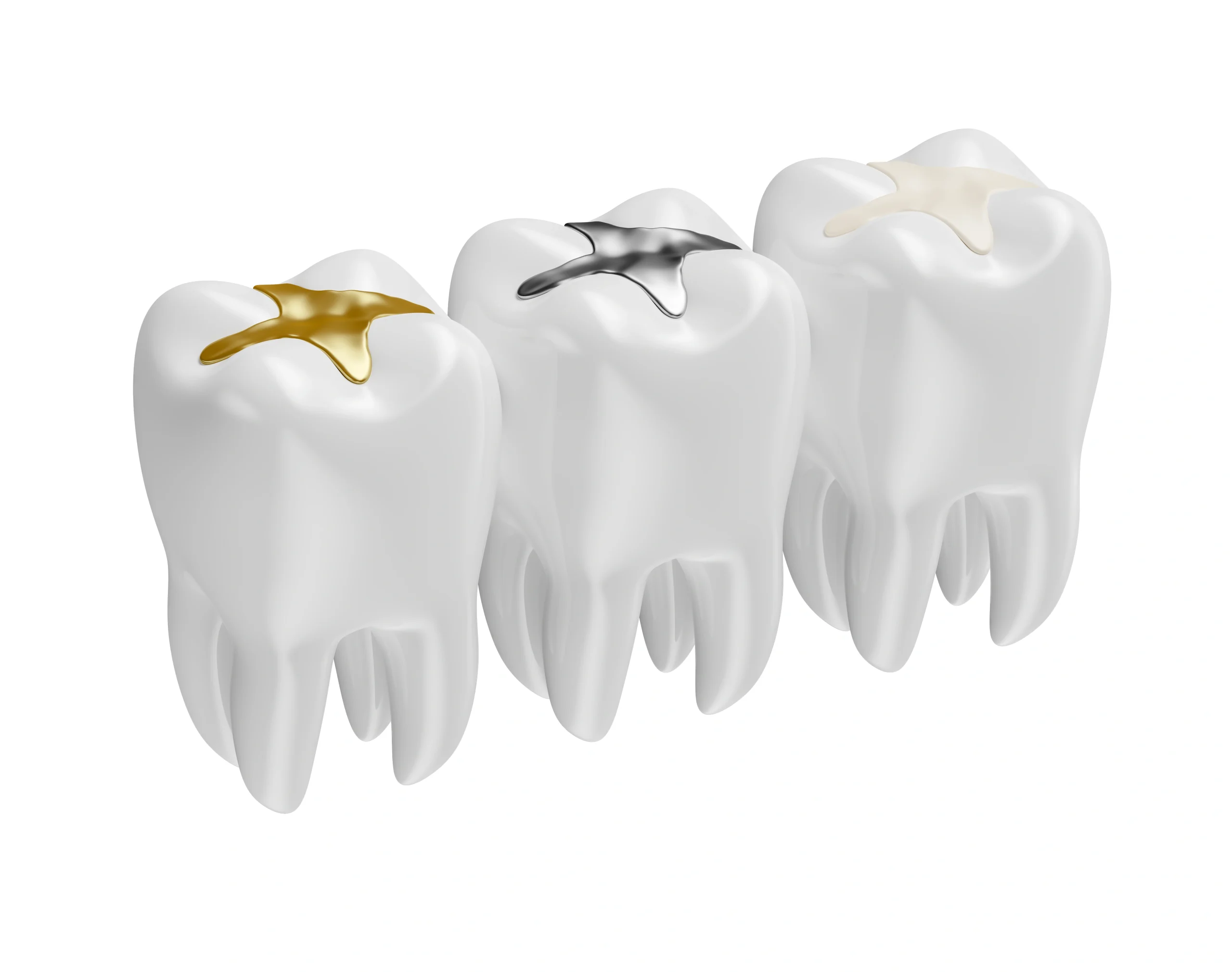
Dental fillings work by sealing the cleaned cavity with a strong, biocompatible material that bonds to the tooth. This creates a protective barrier that blocks bacteria, stops decay from spreading, and restores the tooth’s natural strength.
The material hardens in place, allowing the tooth to regain its shape, stability, and chewing function. By reinforcing weakened areas and preventing food or bacteria from entering, fillings keep the tooth healthy and comfortable for years.
A quick, single-sitting treatment that restores strength, comfort, and a natural smile.







Price Range Per Filling
₹ 850 - 2,450*
Note: ₹1,290 covers a basic composite filling for a single surface. Final cost may vary based on cavity size, number of surfaces, and any additional procedures required. Prices as of August 2025.
High-quality, long-lasting composite materials sourced directly from trusted manufacturers.
Your receipt clearly mentions the filling material, brand, and type used with no hidden costs.
Flexible EMI plans available for larger treatments or multiple fillings, including interest-free options.
Covers diagnosis, filling placement, finishing, and required follow-up, all under one care plan.
Not every cavity can be treated with a simple filling. The right treatment depends on how deep the decay is and how much of the tooth is affected. Here’s a quick guide to help you understand what your dentist may recommend:
| Factor | Filling | Root Canal (RCT) | Crown |
|---|---|---|---|
| Decay Level | Small–moderate cavity | Deep decay near the nerve | Large cavity / weak tooth |
| Pain / Symptoms | Mild sensitivity | Severe or spontaneous pain | Used if tooth structure is weak or damaged |
| Tooth Condition | Tooth structure mostly intact | Swelling or prolonged sensitivity | Cracks or major tooth loss |
Swipe right to see Comparison
Investment Perspective: Though implants have a higher upfront cost, their longevity and health benefits make them the most cost-effective choice over time.
Personalised guidance from Clove’s experienced dentists for safe, painless, long-lasting fillings.

100% Privacy
Your details are safe - no spam.

Expert Dentists
Skilled in cavity diagnosis & tooth-coloured restorations.

Painless & Quick Procedure
Single-sitting, comfort-first approach.

Happy Patients
55K+ cavity cases treated successfully.
All dental fillings are performed under strict infection-control and 4-step sterilisation standards to ensure complete safety, hygiene, and comfort.
Get treated by trained dentists specialising in cavity management and tooth restoration ensuring precise, durable, and natural-looking results.
We use high-quality composite systems, nano-hybrid materials, and minimally invasive techniques for long-lasting, natural looking restorations.
Standardised protocols across 715+ clinics ensure every patient receives uniform, reliable, and high-quality dental care every single time.
With 715+ clinics in 26+ cities, access care anywhere—your records stay digital, clinics are open on weekends, with late appointments available.

Your dentist checks the tooth, identifies the cavity, and explains the treatment plan.
An X-ray is taken in every case to evaluate the depth of decay and ensure the right treatment choice.
The damaged portion of the tooth is gently cleaned out to stop further infection.
Tooth-coloured material is applied and shaped to match your natural tooth.
A curing light is used to strengthen and secure the filling.
Your dentist adjusts the filling for smooth, comfortable chewing.
The restored tooth is polished for a natural, glossy finish.
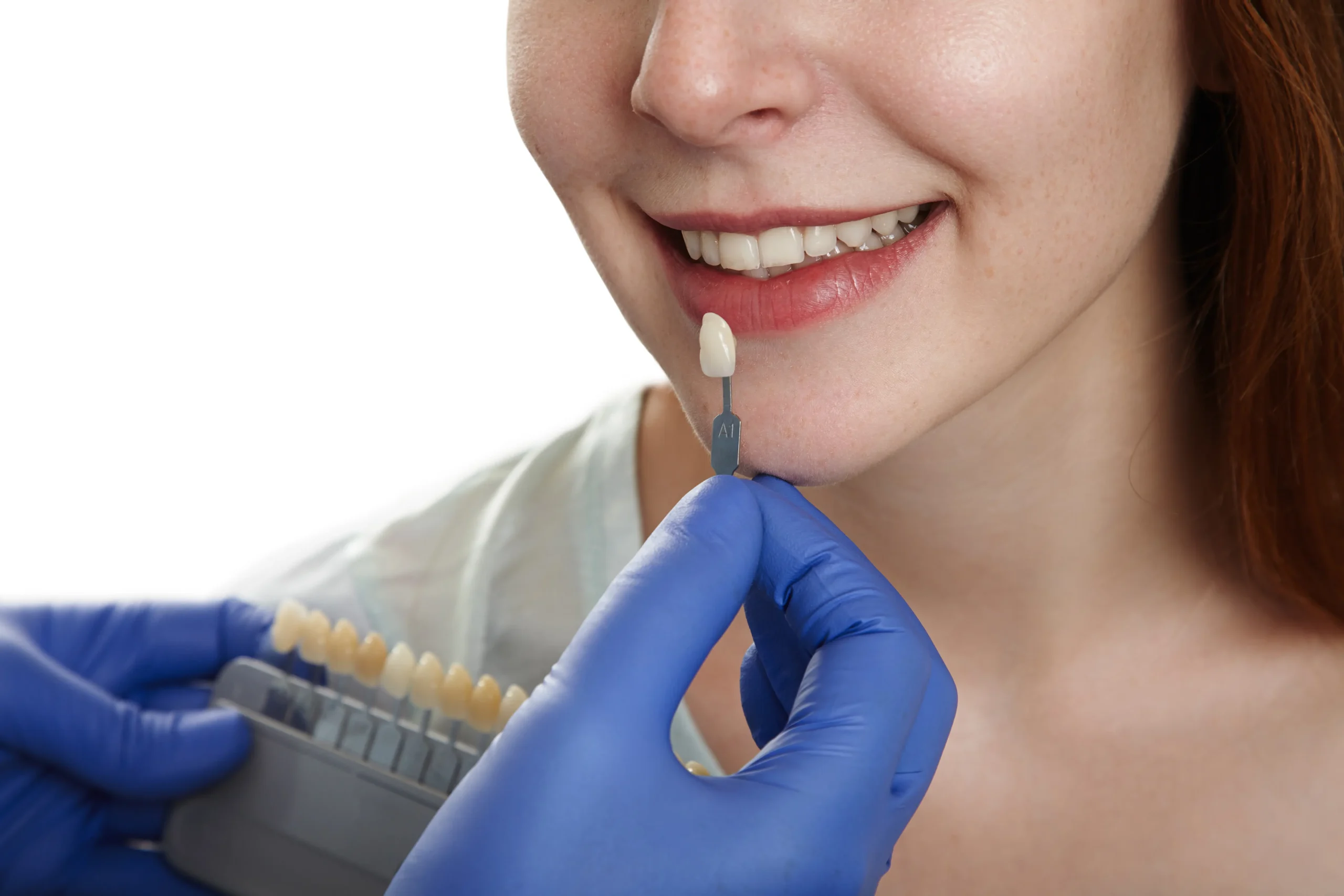
Tooth-coloured material that blends naturally; ideal for most cavities.
Strong, stain-resistant option for long-lasting, aesthetic restorations.
Releases fluoride; suitable for non-load-bearing areas and children’s teeth.
Advanced, high-strength composite for superior polish and durability.
Personalised guidance from Clove’s experienced dentists for safe, painless, long-lasting fillings.

100% Privacy
Your details are safe - no spam.

Expert Dentists
Skilled in cavity diagnosis & tooth-coloured restorations.

Painless & Quick Procedure
Single-sitting, comfort-first approach.

Happy Patients
55K+ cavity cases treated successfully.
Common questions about Dental Fillings
A dental filling restores a tooth damaged by decay, cracks, or fractures. The dentist removes the affected tissue, cleans the cavity, and fills it with a suitable material to restore the tooth’s shape and function. Without a filling, the cavity deepens, reaches the pulp, and eventually requires root canal treatment or extraction.
The main types are tooth-coloured composite resin, glass ionomer, ceramic (inlay/onlay), and silver amalgam. Composite resin is the most popular choice, it matches tooth colour, bonds directly to enamel, and requires less drilling than amalgam. Clove Dental uses tooth-coloured composite as its standard material for both aesthetics and durability.
Signs include toothache, sensitivity to hot or cold, visible dark spots or holes, food consistently getting stuck, or a rough edge you can feel with your tongue. However, early cavities often have no symptoms at all, only dental X-rays can detect them reliably. A 6-monthly check-up at Clove Dental catches cavities before they worsen.
No. Dental fillings are performed under local anaesthesia, so you feel no pain during the procedure, only mild pressure or vibration. Post-procedure sensitivity for a few days is normal and resolves on its own. Clove Dental’s 10x safety protocols and trained dentists ensure a calm, pain-free filling experience across all clinics.
Most dental fillings are completed in a single appointment of 30–45 minutes. The time depends on the cavity’s size, depth, and location. Composite resin fillings cure instantly under a curing light, so you can eat soft foods shortly after. Indirect ceramic inlays require two visits due to laboratory fabrication.
Composite resin fillings last 7–10 years; ceramic inlays can last 15+ years with proper care. Longevity depends on the material, the size of the filling, biting forces, and oral hygiene habits. Regular 6-monthly check-ups at Clove Dental allow dentists to monitor filling integrity and replace them before secondary decay develops underneath.
Real smiles, real stories. Here's what our patients love about their CLOVE Dental experience!

Clove Dental has clinics in 27 cities in India. Find the nearest one for expert Dental Implant care at a reasonable cost.